
Midwives in northern Sierra Leone now have access to portable ultrasound technology, thanks to the Doctors for Development project.
Becoming pregnant in Sierra Leone is a scary prospect. Women here have a one in 17 chance of dying during pregnancy or childbirth – thought to be the highest maternal mortality rate in the world.
It’s not hard to see why. In Bombali District, over 600,000 people rely on just 48 maternal and child health posts. Many are based in rural communities, and are equipped with only the most basic of facilities: a bed, a community health worker and whatever medicines are not currently in shortage.
Midwives under pressure
“We only have very basic things at this unit,” says Catherine Swaray, who has delivered over a thousand babies in five years as a rural midwife.
“At the hospital they can offer comprehensive obstetric emergency care. They can offer blood transfusion, caesarean section, newborn intensive care. We have none of that here. So if we have a complicated delivery it’s important that we know, so that we can refer.”
Catherine’s facility is typical – women with anything but the most straightforward pregnancies could be in mortal danger.
“It's really a matter of time. As soon as you know this case is an emergency, it has a time limit because the baby will not wait for you to get prepared. The longer you stay, the more distressed the baby becomes.”
Sadly, all too often complications are spotted too late - and babies’ lives can't be saved.
Your responsibility is to save the mother and the child. And if the child dies, you did not do your job for the mother.Catherine Swaray, midwife
“When we lose a baby, I have to shed tears. I'm a mother, too. I have three children. I know how it feels. Most times you do not cry in front of them. I will just go to my office, because it tells on you as the midwife. Your responsibility is to save the mother and the child. And if the child dies, you did not do your job for the mother.”
Maternal health inequalities
The pressures faced by midwives like Catherine are incredible, especially when considered in the context of the discrepancies between rural Sierra Leone and wealthier countries.
The WHO recommends an ultrasound scan in the first 24 weeks of pregnancy to detect foetal abnormalities, complications and multiple pregnancies – which could help midwives make important decisions.
It’s something taken for granted by expectant parents living in wealthier parts of the world: having a scan is a ritual that provides reassurance, peace of mind and an opportunity to connect with the life growing inside them. Seeing their baby’s heartbeat on the ultrasound monitor for the first time is a moment few mothers forget.

This is not the experience, however, for the vast majority of women in Bombali district, Sierra Leone. Just one single ultrasound machine exists in Makeni General Hospital, a facility serving an area of nearly 8,000 km2 that is home to well over half a million people.
Most live in rural locations far from the hospital, relying on a basic health centre, which may still be hours away from home.
Making maternity care mobile
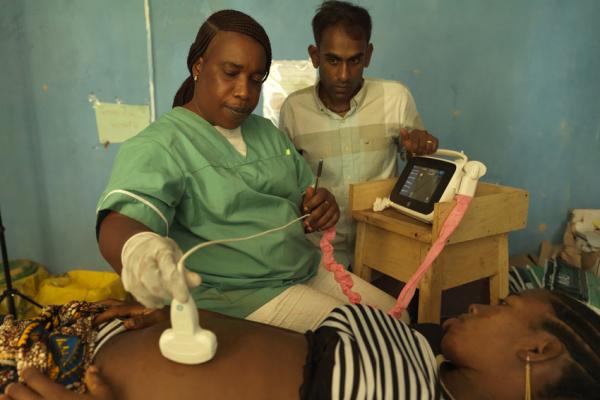
Thankfully, things are changing. The Doctors for Development project has provided portable ultrasound machines, known as V-scans, for the very first time in northern Sierra Leone. Midwives have been trained to use the technology, which is allowing them to spot complications early, and, crucially, to refer expectant mothers to hospital to reach specialist care - before it’s too late.
The fact that the V-scan is portable means that the midwives trained to use it can cover a wide area, traveling all over the Bombali district providing regular antenatal clinics to women, no matter how far they live from maternal health facilities.
When midwife Catherine passes through a rural village on the back of a motorbike, ultrasound scanner kit slung over her shoulder, pregnant women hurry to join her, calling each other to join for a scan.
She’s assisted by VSO volunteer Dr Kiran Cheedella, whose role includes mentoring and coaching rural midwives and community health workers on effective use of the V-scans.
At one such clinic at Kamaranka, women in various states of pregnancy line up for a check, which will include a scan, as well as tests for blood pressure and blood sugar levels.
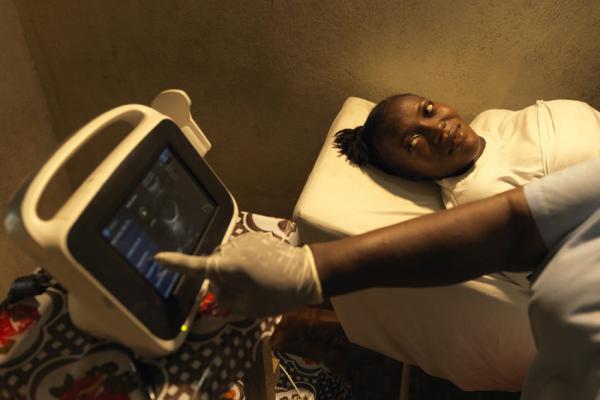
Though the technology is new to these women, they are excited and happy to receive expert medical attention.
Mamie Momoh, 21, has just seen her baby for the first time, and heard she is due to deliver a healthy child very soon: “I saw my child! It's like a video. And the nurse told me that my baby's head is now pointing down, it's ready. I was so happy seeing my baby. The only thing I was unable to know is whether the baby is a boy or a girl. I am excited to find out!”
Volunteer Kiran is hopeful for this work, and the potential for expansion:
"I’ve seen a huge increase in knowledge of the midwives and their ability to scan well. It’s really been impressive to see how well they’ve done in these few months and also on how much they’ve taken it on as a duty to themselves, to go out there and find other health care centres, not just remaining attached to their own. To try and get there to scan more and more women, they’re really getting into it and excited to scan and I think they’re going to create a really big impact in the community.”
Find out more about our work in:

Sierra Leone
We've worked in Sierra Leone for over 50 years, building healthy communities and supporting people to develop secure and resilient livelihoods.

