In Malawi, one child in eight dies before reaching age of five, often because of poor access to qualified health workers.
Through the Tropical Health & Education Trust (THET) programme, UK nurse trainer David Atherton is spending just under two years at a hospital in rural Malawi sharing vital nursing skills with more than 100 students.
Addressing the chronic shortage of trained health professionals is seen as key to help directly reduce the number of people dying because of inadequate access to professional healthcare.

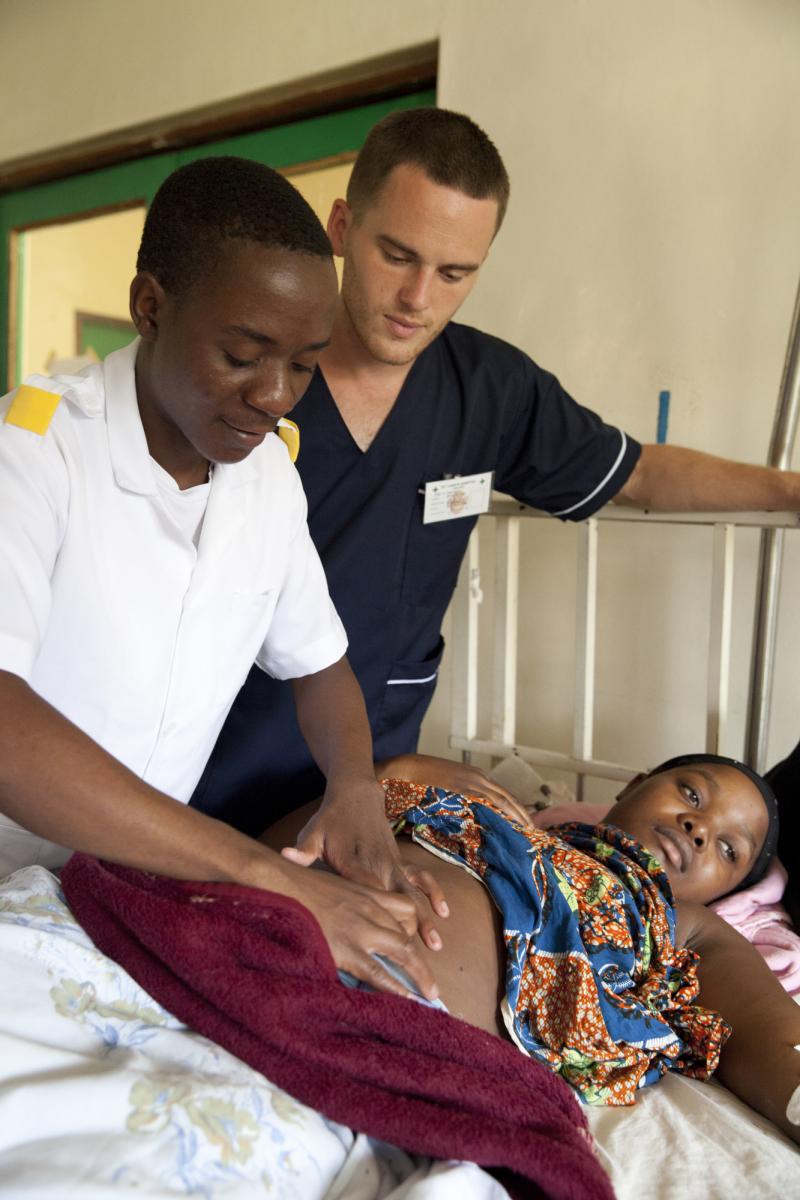
David Atherton, THET programme VSO volunteer at work in St Lukes Hospital, Zomba district, Malawi.
What made you decide to do VSO?
I’ve always wanted to do VSO; my mother did VSO 50 years ago in Papua New Guinea; so I’ve always known about the organisation. I was also keen to do something that involved using my health skills and education, so training nurses through VSO seemed ideal.
Can you describe what you are doing in Malawi?
I’m training student nurses at a nursing college attached to a rural hospital called St Luke’s, near the city of Zomba. I train over a hundred students who are undergoing a three-year training programme to qualify as ‘Nurse Midwife Technicians’.
The training involves covering the theory in a Skills Lab and also overseeing clinical training of nurses on hospital wards.
Nursing students Diana Liphana and Stevien Saiwala peer teach each other at St Lukes hospital, Zomba district, whilst their mentor David Atherton, VSO volunteer and THET programme nurse clinical instructor watches
What are the major health issues you see in Malawi?
There’s a real shortage of trained health workers in Malawi. You find nurses are qualified at different levels, and often those in village health centres have very basic skills, so it’s only when you get to hospital that you find registered qualified nurses.
85% of Malawians live in rural areas, so there is very poor access to professional healthcare for the majority. Even though St Luke’s Hospital where I am based is in a rural area, it isn’t really regarded as rural because people from surrounding villages will travel a long way to get to hospital, often travelling for hours by foot or bicycle.
What is it like being a nurse in Malawi?
The role of a nurse in Malawi is very complex, because often they have to work at a much higher level than what is typical in the UK, and nurses generally have much more responsibility over aspects of care. Nurses in Malawi are not specialised and based in specific hospital departments, so they’re expected to cover lots and lots of diseases, body systems, admissions and assessments and often have to perform tasks with limited understanding.
I’ve seen how nurses can miss some of the basic things because they’re always thinking about the higher level assessments.
Can you give an example of a simple skill you’ve shared?
I’ve helped introduce ‘head to toe’ examinations for babies when their mothers bring them in for free immunisations at the under-five clinic at St Luke’s Hospital.
The ‘head to toe’ examination is a really important low-cost way of being able to diagnose so many potentially life-threatening issues by identifying simple things like looking at how pink a child’s conjunctiva is, to diagnose early anaemia.
In a place where resources are very scarce, it’s a good way to save money and save lives. The nurse students are quite impressed that we don’t always need to use lots of diagnostic tools or equipment to do our jobs well.
What is it like working with Malawian nurses?
The Malawian students have a yearning for learning and are very enthusiastic and hard working, so it’s a pleasure to work with them.
But there is a hierarchy in Malawi so if a student doesn’t know how to do something, they will often be afraid to ask.
In the UK, we have much more informal relationships with teaching staff, so that is a key difference. During the past few months, I’ve had some really good experiences with students telling me they’ve learnt a lot because they’ve felt confident to say when they didn’t know how to do something.
What are some of the challenges you’ve faced?
I think one of my main issues when I first arrived was to understand how my work could be sustainable. For me, that has come not just by looking for what student nurses or the hospital needs but by encouraging the students to come up with projects and enabling them to highlight what they want to learn or improve at the hospital.
I feel this makes a big difference, as the student nurses not only feel a sense of ownership over such work, they also take it forward afterwards.
What have you gained professionally from your one year in Malawi?
Back in the UK, I would never get the breadth of experience I’ve had in Malawi.
I’ve worked clinically on the wards, prepared exams, developed the curriculum and taught in classrooms – sometimes with classes of around 160 students!
I think I’ll be in a much better position to deal with patients from different countries and cultures back in the UK, and also to cope with more diagnosis and problem solving in a clinical setting, something I’m keen to further when I get home.
I’ve also had the opportunity to sit in on meetings at quite high levels so it’s been a really good, broad experience for me.
Do you feel you can really make a difference?
I think it’s really hard to measure how you make a difference as a volunteer, but I think you see it personally when you’re working one on one with students or in groups.
Sometimes you teach a student nurse a skill and wonder ‘did they really understand that?’ and then you’ll later observe one of the nursing students doing exactly what you taught them and doing it perfectly, so yes you do get to see the results.
Ensuring skills stay in Malawi
22 year old student nurse Diana is in her first year of training as a nurse and midwife technician working alongside David.
She is now implementing the ‘top to toe’ examinations during the immunisation clinic, “I was inspired by the work of nurses when I was a little girl – so I studied hard in school to achieve my goal of becoming one,” she recalls.
Much of Diana’s passion for nursing stems from witnessing the health challenges in Malawi’s villages firsthand. “When a child from my village is sick, the women always seek traditional medicine before going to the clinic or hospital and I have seen many children die because they are not treated in time.” In particular, Diana feels she has really learnt how to put theory into practice, and understand how to address more than what the patient feels they need, “By doing the top to toe checkups I have been able to identify other serious problems that the mother did not know her baby had,” she says.
Reflecting on his skills sharing role, David believes expensive equipment and fancy tools aren’t always essential to be a good nurse. He explains, “When we do the top to toe examinations with the students, one of the things they’re quite impressed by is that we don’t use lots of diagnostic tools and equipment...yet it’s a really important and low cost way to diagnose conditions. In a place like Malawi where money and resources are very scarce, it’s a simple way of using skills to save lives.”

David Atherton with his students Diana Liphana and Stevien Saiwala. David, THET programme VSO volunteer at work in St Lukes Hospital, Zomba district, Malawi
What would you say to someone who’s thinking of doing VSO?
When you’re in the UK working the same old routine you can get stuck in a bit of a rut, so volunteering overseas definitely offers you an exciting and refreshing experience.
I think you’ve got to have an adventurous spirit and understand there will be frustrations but balancing that out there’s so many exciting experiences to have and brilliant relationships to build.
Volunteering just kind of extends your life and gives you extra years to put in between, so I would say to anyone thinking of doing VSO, just go for it.
Interested in volunteering?
Find out more about volunteering, working in Malawi, or check out our latest volunteer jobs.
